When we think of osteoporosis we think about frail elderly ladies who are bent and have trouble walking. But what is osteoporosis?
What is osteoporosis?
Osteoporosis is the gradual loss of bone density due to deterioration of bone tissue. This loss of bone density causes bones to be frail and puts the individual at risk of suffering a fracture. This conditions is considered a “silent pathology”. Someone who has osteoporosis will not experience pain or symptoms. Many people do not even realise they have osteoporosis until they suffer a fractured or broken bone. The area’s of the body most commonly affected by osteoporosis include the hip, wrist, and vertebral bodies of the spine.
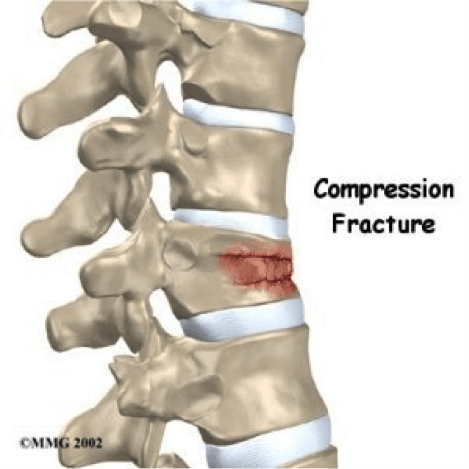
A compression fracture in a vertebral body.
People who have had radiotherapy, prolonged use of steroids, early menopause or total hysterectomy may be at a higher risk of osteoporosis than the general population. Lifestyle factors including:
- low levels of physical activity
- high intake of alcohol and smoking
- poor diet or a history of eating disorders,
may also increase the risk of developing osteoporosis.
What can you do?
Increasing exercise levels is an effective management strategy for osteoporosis. It is recommended that a person suffering from osteoporosis does a variety of loading exercises. There are no fixed rules, but walking or running, strength training, postural and balance exercises (all weight bearing exercises) are all useful for the management of osteoporosis and the prevention of fractures. It has been shown that regular weight bearing and strengthening exercises loads the bones, increases bone density and reduces the effect of osteoporosis. However, inappropriate exercises may increase the risk of fractures once osteoporosis has developed. It is therefore important to consult with a qualified professional, such as a physiotherapist prior to beginning an exercise program.
What kind of exercises?
Studies looking at exercise and osteoporosis have compared a spinal flexion (bending forwards) program to a spinal extension (bending backwards) program. Spinal flexion has been shown to increase the load through the vertebral bodies of the spine (which is most commonly affected by osteoporosis and therefore at highest risk of fracture). Spinal extension promotes improved posture, increased load through the pedicles of the vertebrae and therefore less load through the vertebral bodies.
One study compared 4 groups of individuals with osteoporosis.
- Group 1 completed only extension based exercises: 16% suffered a wedge or compression fracture
- Group 2 completed only flexion based exercises: 89% suffered a wedge fracture
- Group 3 completed both flexion and extension based exercises: 53% suffered wedge fractures
- Group 4 did not exercise: 67% suffered a wedge fracture
This study clearly highlights that exercise can be effective in reducing the risk of fractures associated with osteoporosis. It also demponstrates the importance of an appropriately prescribed exercise program for the management of osteoporosis and shows how exercise can be used in the management of osteoporosis and to prevent spinal fractures.
Disability associated with osteoporosis often occurs as a result of a fall, therefore falls prevention programs are another important part of the management strategy for this condition.
Would you like to know more?
For further readig on this subject we recommend the following articles (let us know if you need assistance in accessing these):
- Postmenopausal Osteoporosis: Flexion vs Extension exercises, M Sinaki, Mikkelsen, Archives Phys Med Rehabilitation, 1984, Vol 65
- Balance disorder and increased risk of falls in osteoporosis and kyphosis: significance of kyphotic posture and muscle strength, M Sinaki, R Brey, C Hughes, D Larson, K Kaufman, Osteoporosis International, 2005, Issue 16, Pg 1004-1010
- www.betterhealth.vic.gov.au/health/conditionsandtreatments/osteoporosis
More exercise ideas?
Look at our fabulous blog posts on walking, stretching, or if you are really energetic (and don’t have any disorders that make exercising at a high level dangerous) our HIIT program.






