A patellofemoral dislocation is a common injury where your kneecap dislocates from the knee joint. In lay terms, your knee cap is no longer where it is supposed to be…
Patellofemoral dislocation occurs more commonly as a sports injury, but 40% of the time, in non sports scenarios. In post instances, the kneecap predominantly dislocates to the outside of the knee when the knee is bending and can be either a traumatic (in an accident or incident) or non-traumatic injury (when you are minding your own business and it jumps seems to pop out of place.

Patellofemoral Joint
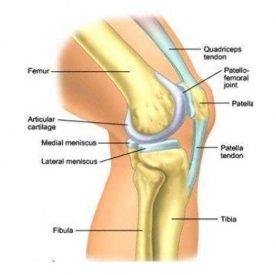
The patellofemoral joint is the site where your kneecap articulates or makes contact with your femur (thigh bone) and tibia (shin bone) that lie beneath the knee cap. A dislocation occurs when the kneecap “slides off” to the side of these bones. The knee will look unusual and you will experience pain.
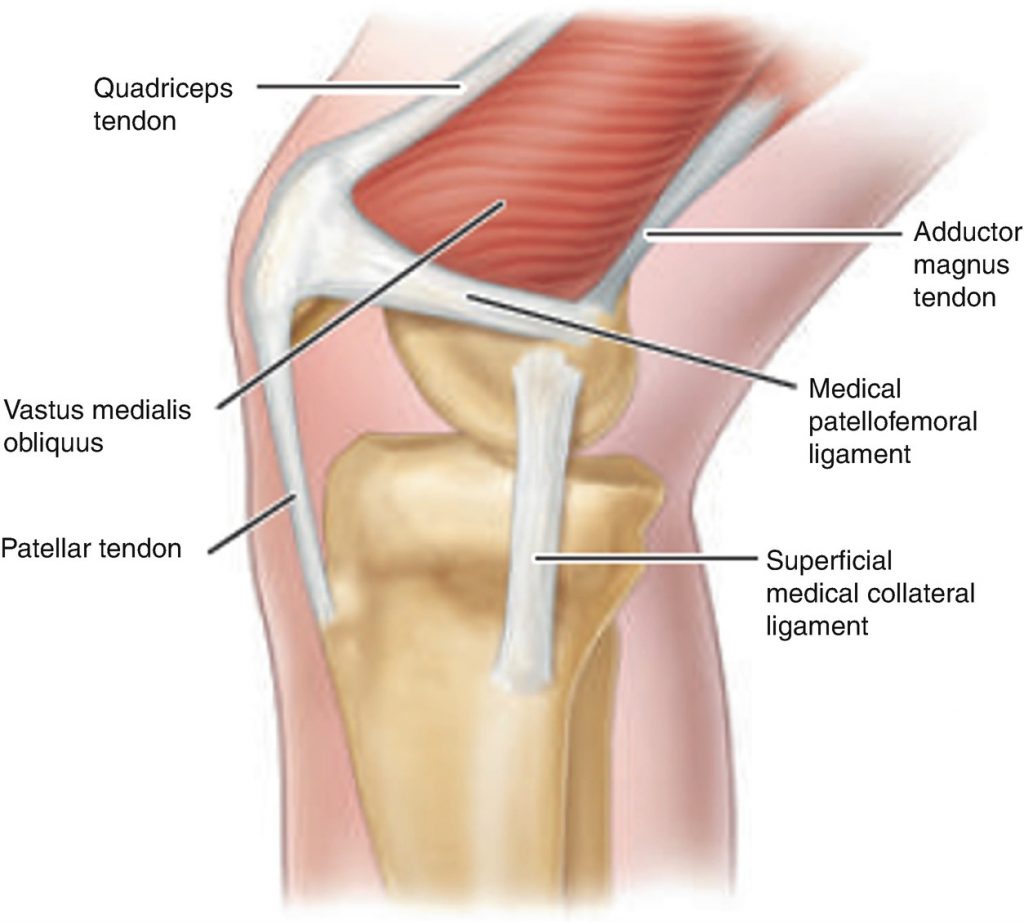
During this injury, the Medial Patellofemoral Ligament (MPFL) is torn which can be an ongoing source of pain and instability if it isn’t allowed to heal properly as this ligament accounts for up to 60% of kneecap stability.
What to Expect (Symptoms)
Most patients describe a “pop” or “snapping” sensation when they dislocate their knee, and occasionally the kneecap will partially dislocate and then slide back into place. Sometimes if the kneecap slides back into place it can be hard to know exactly what just happened!
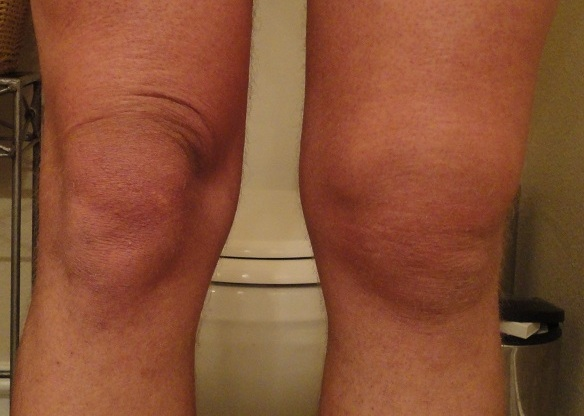
If your knee has dislocated there are several symptoms that can occur which will depend upon the severity of the injury, including:
- Anterior knee pain (pain in the front of the knee
- Swelling (can be a lot!)
- A feeling of instability or lack of trust in the knee when walking
- Apprehension and an unwillingness to extend the knee
Early Management
If you have dislocated your knee you are likely to be experiencing significant pain and swelling. This is of course depending upon the severity of your injury and if there was any other injury to the knee that occurred during the injury. (Your physiotherapist will be able to provide you with more information about this when they assess your knee).
Early assessment and management is important as a history of kneecap dislocations can increase your chance of re-injury in the future if the injured structures, such as the MPFL, are not allowed to heal correctly.
To allow the MPFL ligament to heal the movement within your knee needs to be controlled. This is achieved through the use of a ROM brace for 6 weeks
During this stage you will be asked to commence both strengthening and range of motion exercises to start working towards rehabilitation.
Do I Need a Scan?
The mechanism that causes a knee dislocation is similar to the mechanism that can cause damage to your meniscus, ligaments and even bone within the knee. To check for this:
- An x-ray is useful in immediately ruling out any additional injuries to the bone such as fractures that will need to be addressed.
- Depending on how you dislocated your knee, an MRI may also be required to assess the soft tissue within your knee for injury.
Rehabilitation
Physiotherapists use a range of tools and treatments to guide you through a staged rehabilitation program that will see you safely returned to your sport and daily life. Some of these management strategies include:
- Education on pain medications and potentially anti-inflammatories (if your GP advises that you are safe to take them)
- Taping to support the knee
- Manual therapy to assist with pain and swelling
- Ice for pain management
These techniques are used in combination with a slow, graded exercise program that is tailored specifically to your sport and broadly includes:
- Range of motion exercises to achieve full range
- Quadricep Strengthening for your inner quads to achieve knee stability when walking
- Global lower limb strengthening to address any strength losses from the brace
- Targeted quadriceps strengthening
- Sport specific retraining including cutting, pivoting, landing, plyometrics, single leg stability
Knee rehabilitation following dislocation is often a 12-week process and it is extremely important to retrain your knee following injury to confidently and safely return to play.
If you, or someone you know, requires an assessment or advice please don’t hesitate to contact us today!
References
- Parikh, S., Lykissas, M., & Gkiatas. (2018). Predicting risk of recurrent patella dislocation. Curr Rev Musculoskeletal Med. 11(2): 253-260. doi: 10.1007/s12178-018-9480-5
- Orthobullets. (2020). Patella Instability. https://www.orthobullets.com/knee-and-sports/3020/patellar-instability
- Rhee, S., Pavloa, G., Oakley, J., Barlow, D., & Haddad, F. (2012). Modern management of patella instability. 36(12): 2447–2456. doi: 10.1007/s00264-012-1669-4
- Menetrey, J., Putman, S., & Gard, S. (2014). Return to sport after patellar dislocation or following surgery for patellofemoral instability. Knee Surg Sports Traumatol Arthrosc. 22(10): 2320–2326. doi: 10.1007/s00167-014-3172-5
- Hinton, R., & Sharma, K. (2003). Acute and recurrent patellar instability in the young athlete. Orthop Clin North Am. 34(3):385-96.
- Mochizuki, T., Tanifuji, O., Sato, T., Watanabe, S., Omori, G., & Endo, N. (2020). Scoring system for optimal management of acute traumatic patellar dislocation: A multicenter study. Journal of Orthopaedic Science. 25(1): 173-177.
- Jain, N., Khan, N., & Fithian, D. (2011). A Treatment Algorithm for Primary Patellar Dislocations. Sports Health. 3(2): 170–174. doi: 10.1177/19417381113992374
- How’s Health. (2020). Swollen Knee [Image]. Retrieved from https://howshealth.com/swollen-knee-symptoms-causes-treatment/
- Rugby Strength Coach. (2020). Rugby Side Step [Image]. Retrieved from https://rugbystrengthcoach.com/rugby-performance/side-step/
- Sydney Knee Specialists. (2020). Knee Anatomy [Image]. Retrieved from http://www.sydneyknee.com.au/medial-patellofemoral-ligament-reconstruction/







