What Is Osteoarthritis?
Osteoarthritis (OA), also known as osteoarthroses, is a type of degenerative joint disease. OA is a disease of the entire joint, encompassing the cartilage, joint lining, ligaments and bone. Although it is commonly referred to assimple ‘wear and tear’, there is much more to the disease, with cartilage breakdown, bony overgrowth and alterations to ligaments,menisc and muscles surrounding the joint. As the role of cartilage is to cushion the ends of bones within joints, when the cartilage breaks down there is contact between each end of the bones. Importantly – improvements in strength and flexibility can improve pain levels and function.
What is the cause?
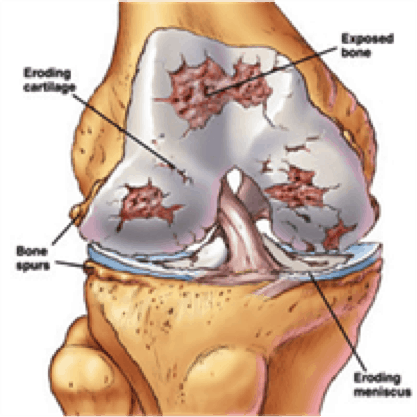
Osteoarthritis of of the Knee
The cause of OA is not yet known, however it can be associated with mechanical stress and biomechanical alterations, as well as genetic factors. As the knee is significantly required for weight bearing during daily activities there is a higher incidence of OA affecting this joint.
What are the symptoms?
- Decreased function of the knee
- Joint pain and stiffness
- Swelling at the joint
- Cracking, grinding noise or ‘catching’ with joint movement
- Bony growths at the margins of affected joints
Who Gets Osteoarthritis?
Most often OA occurs in patients over the age of 40 however, it will sometimes affect someone before this age if they have additional risk factors. Risk factors include:
- Family history of OA
- Older age
- Obesity
- Joint or nerve injury
- Repetitive use of the knee
- Joint deformity: bowlegs, knock knees, or unequal leg length
- Lack of physical activity
- How Is it Diagnosed?
Although the patient’s medical history and symptoms are often enough to distinguish the presence of OA, the patient may be required to have a magnetic resonance image (MRI) or X-Ray to grade the extent of the disease or rule out other contributors. Joint aspiration will be conducted to rule out other forms of arthritis within the body.
How is Osteoarthritis Treated?
Although there is no cure or way of reversing the joint damage, treatment is aimed at reducing pain and improving function of the knee. Treatment includes:
- Physical activity: this will maintain joint flexibility and strength of surrounding muscles while assisting with weight reduction. Strengthening exercises are a scientifically proven strategy for managing osteoarthritis.
Strengthening exercises are a scientifically proven strategy for managing pain and disability from osteoarthritis.
- Weight Control: is required for prevention and to slow the progression of OA affecting the knees.
- For every 0.5 kg of weight lost, there is 2 kg reduction in the load exerted by the knee for each step taken during daily activities.
- Losing as few as 5 kg can cut the risk of developing knee OA by 50% for some women
- Weight loss of only 7 kg can cut knee pain in half for overweight individuals with arthritis.
- Joint Protection: to prevent further strain and stress on the knee joint with use of braces, canes and shoe inserts.
- Medication: can be used to relieve pain, swelling and stiffness to allow the patient to once again become physically active.
- Dietary supplements such as glucosamine and chondroitin sulphate have been shown in cases of severe OA to reduce pain and improve joint function
- Surgery: is a consideration when the damage from the OA has significantly progressed causing the patient to be limited in their function.
Physiotherapy
Physiotherapy has an important role in the management of OA. In addition to assisting with drug free management of acute episodes of pain, physiotherapy can tailor:
- a strength program to ensure maximum strength of the supporting structures around the knee;
- a flexibility program to ensure that tight muscles are not working inefficiently and resulting in higher pain levels.
Call us to discuss.
Useful links
Reference
K.L. Bennell, R.S. Hinman / Journal of Science and Medicine in Sport 14 (2011) 4–9







